Introduction: When Physical Symptoms Carry Emotional Weight
Chronic vascular conditions are often discussed in strictly medical terms. Swelling, aching legs, visible varicose veins, skin discoloration, and reduced mobility are viewed as physical manifestations of circulatory dysfunction. Yet for many individuals, the emotional burden of these conditions can be just as significant as the physical discomfort. Living with a long-term vascular disorder frequently affects confidence, social participation, work performance, and overall quality of life. As digital health technologies evolve, an important question is emerging: can artificial intelligence detect the hidden emotional distress that often accompanies chronic vascular disease?
Understanding the psychological dimensions of vascular health requires a broader perspective. Conditions such as chronic venous insufficiency and varicose veins are not merely cosmetic concerns. They can represent ongoing pain, fatigue, and limitations that quietly reshape daily life. The integration of AI-driven emotional analytics into healthcare may offer new opportunities to identify and address distress before it becomes overwhelming.
Chronic Vascular Conditions and Their Daily Impact
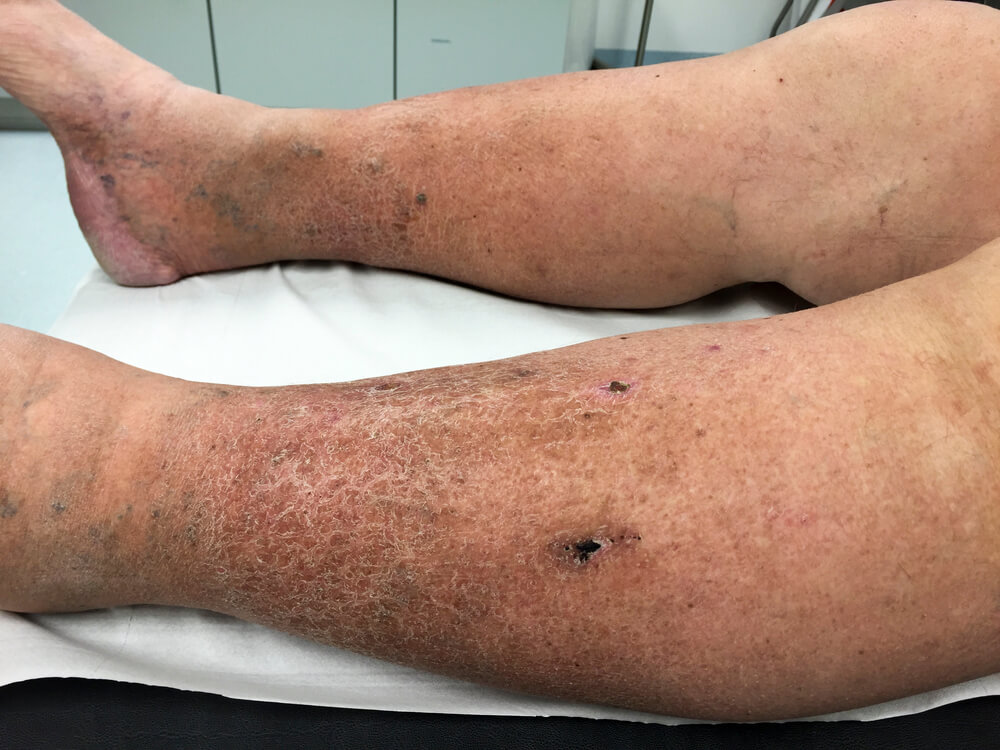
The vascular system plays a vital role in maintaining tissue health by transporting oxygen and nutrients throughout the body. When venous valves weaken or blood flow becomes impaired, pressure builds in the lower extremities. Over time, this can result in visible varicose veins, persistent swelling, heaviness, and skin changes. While these symptoms may appear manageable from a clinical standpoint, their cumulative effect can be profound.
Patients often describe a gradual narrowing of their world. Activities that once felt effortless, such as standing for extended periods or participating in social gatherings, may become exhausting. Some individuals modify clothing choices to conceal visible veins. Others avoid events altogether due to discomfort or embarrassment. These subtle behavioral shifts can lead to isolation, frustration, and diminished self-esteem. The emotional impact may remain unspoken during medical appointments focused primarily on physical findings.
The Psychological Toll of Visible and Persistent Symptoms
Chronic conditions carry a psychological dimension that extends beyond pain. When symptoms are visible, as in the case of prominent varicose veins, body image concerns frequently arise. Individuals may internalize negative perceptions about their appearance, leading to reduced confidence and heightened self-consciousness. For professionals whose roles require prolonged standing or public interaction, visible vascular issues can feel particularly distressing.
Beyond appearance, the unpredictability of symptoms contributes to anxiety. Flare-ups, increased swelling after long workdays, or persistent discomfort can create a sense of uncertainty. Patients may worry about progression, potential complications, or the need for medical procedures. This ongoing vigilance activates stress responses that affect sleep, mood, and cognitive clarity. Over time, emotional strain can compound physical discomfort, creating a cycle in which stress exacerbates inflammation and pain perception.
Hidden Distress in Clinical Settings
One of the challenges in managing chronic vascular disease is that emotional distress often remains hidden. Patients may downplay psychological symptoms during consultations, focusing instead on measurable physical concerns. Cultural expectations and personal beliefs can further discourage open discussions about anxiety or sadness related to medical conditions.
Healthcare providers are trained to assess physical indicators such as vein diameter, skin integrity, and edema. However, subtle cues of emotional strain may be overlooked. A patient’s tone of voice, hesitations, facial microexpressions, or shifts in speech patterns can reveal underlying stress that is not explicitly stated. Identifying these signals consistently across large patient populations is difficult without technological support.
The Rise of AI in Emotional Analytics
Artificial intelligence has begun transforming healthcare through predictive modeling, diagnostic imaging analysis, and personalized treatment planning. A newer frontier involves emotional analytics, where AI systems analyze vocal characteristics, speech patterns, facial expressions, and behavioral data to detect emotional states. By identifying markers of stress, depression, or anxiety, AI tools may assist clinicians in recognizing distress that might otherwise go unnoticed.
Voice-based AI systems can evaluate subtle variations in pitch, tempo, and energy. Research suggests that emotional states influence vocal biomarkers, providing measurable indicators of psychological strain. Similarly, computer vision technologies can detect microexpressions associated with sadness or anxiety. While these tools do not replace clinical judgment, they offer supplementary insights that may enhance holistic care.
Applications in Chronic Vascular Care
In the context of chronic vascular conditions, AI-driven emotional detection could serve as an early warning system. For example, telehealth consultations increasingly involve video interactions. AI platforms integrated into telemedicine software could analyze speech and facial cues during virtual visits, flagging potential emotional distress for further discussion. This approach encourages proactive conversations about mental health without placing the burden solely on patients to initiate them.
Additionally, wearable technologies that monitor physiological indicators such as heart rate variability may provide indirect markers of stress. When combined with patient-reported symptom data, AI algorithms can generate comprehensive profiles of both physical and emotional well-being. For individuals seeking medical solutions such as Vein Treatment in Allen Park, integrating emotional assessments into vascular care may lead to more personalized treatment plans.
Ethical Considerations and Patient Privacy
The use of AI in emotional detection raises important ethical questions. Patients must be informed about how their data is collected, analyzed, and stored. Transparency and consent are fundamental to maintaining trust. Emotional analytics should never be used to label or stigmatize individuals but rather to support compassionate intervention.
There is also the risk of overreliance on technology. AI tools should augment, not replace, human empathy. A clinician’s attentive listening and genuine concern remain irreplaceable components of effective care. When implemented responsibly, AI can serve as a supportive resource that enhances clinical awareness rather than diminishing personal connection.
Integrating Emotional Awareness into Vascular Treatment Plans
Recognizing emotional distress is only the first step. Effective integration requires coordinated care that addresses both physical and psychological dimensions. Vascular specialists can collaborate with mental health professionals to provide comprehensive support. Even brief screening tools for anxiety and depression can make a significant difference when incorporated into routine vascular evaluations.
Patients benefit when healthcare providers acknowledge the emotional realities of chronic illness. A simple conversation about how symptoms affect daily life can validate experiences that might otherwise feel isolating. When treatment plans include both medical interventions and supportive resources, outcomes often improve. Addressing distress may enhance adherence to compression therapy, follow-up appointments, and lifestyle modifications.
The Human Element in a Technological Era
While AI holds promise for detecting hidden distress, technology alone cannot resolve the emotional impact of chronic vascular disease. Compassionate communication, patient education, and empowerment remain central to healing. Individuals who understand their condition and feel supported in managing it are more likely to experience improved well-being.
The future of healthcare lies in blending advanced analytics with human-centered care. AI can identify patterns and subtle signals at scale, but it is the clinician who interprets these insights within the context of a patient’s lived experience. For those navigating chronic vascular conditions, this integrated approach offers hope for more comprehensive and empathetic treatment.
Conclusion: Toward a More Holistic Model of Care
Chronic vascular conditions extend beyond physical symptoms, influencing emotional health in ways that are often invisible. Anxiety, reduced self-esteem, and social withdrawal can quietly shape the patient experience. As artificial intelligence advances, its capacity to detect hidden distress offers a promising avenue for earlier intervention and more personalized care.
However, technology must be implemented thoughtfully, with attention to ethics, privacy, and human connection. By integrating AI-driven emotional analytics into vascular care, healthcare providers can better recognize the full spectrum of patient needs. Ultimately, the goal is not merely to treat veins, but to support the whole person. In doing so, modern medicine moves closer to a future where physical and emotional health are addressed with equal attention and respect.