Chronic diseases such as diabetes, heart disease, and cancer often dominate global health discussions. Yet, beneath the surface of these widely recognized conditions lies another persistent and widespread disorder that affects millions worldwide: Chronic Venous Insufficiency (CVI). Despite its prevalence, CVI frequently goes undiagnosed, misunderstood, or dismissed as a cosmetic concern rather than a significant medical issue. In reality, it represents a substantial burden on healthcare systems and dramatically impacts quality of life for people across continents.
As populations age, lifestyles become increasingly sedentary, and obesity rates rise, the global footprint of chronic venous disorders continues to expand. Understanding CVI as a serious vascular condition rather than a minor inconvenience is essential to improving early detection, prevention, and treatment outcomes.
Understanding Chronic Venous Insufficiency
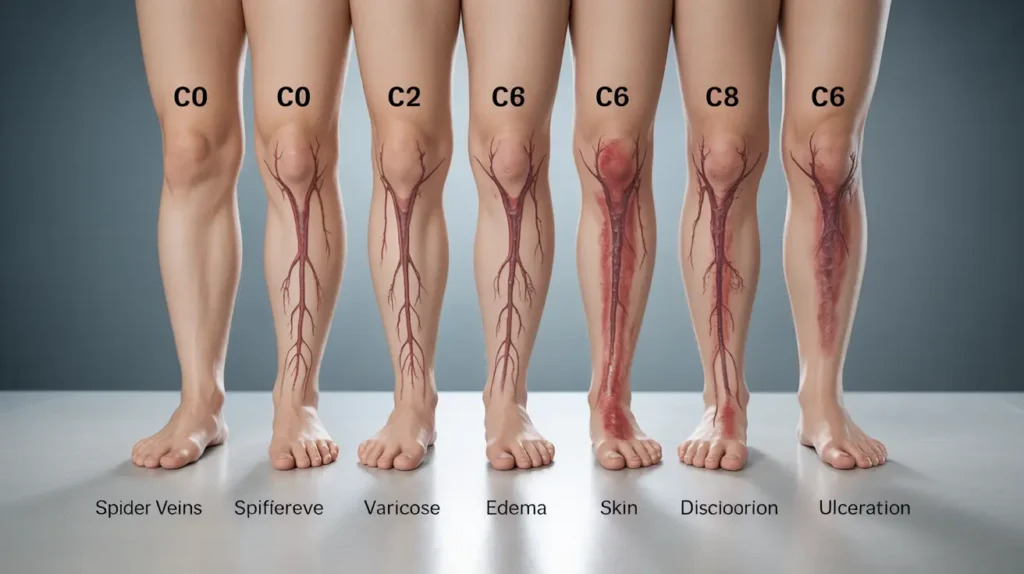
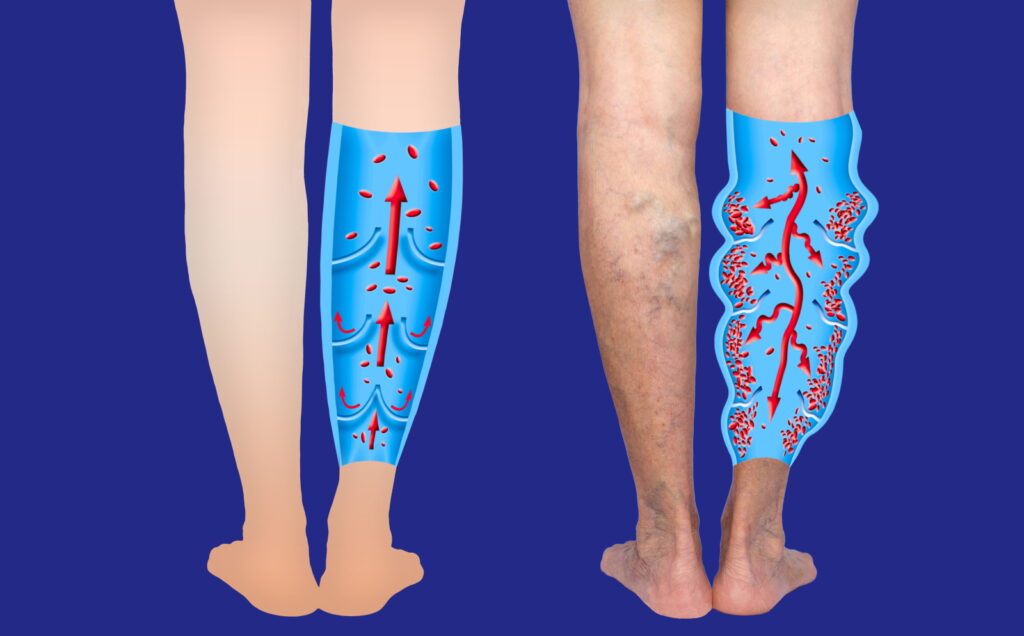
Chronic Venous Insufficiency occurs when the veins in the legs cannot efficiently return blood to the heart. Healthy veins rely on one-way valves that prevent blood from flowing backward. When these valves weaken or become damaged, blood pools in the lower extremities, leading to increased pressure within the veins. Over time, this pressure causes structural changes in the vein walls and surrounding tissues.
The condition often develops gradually. Early signs may include leg heaviness, mild swelling, or visible varicose veins. As the disorder progresses, individuals may experience persistent edema, skin discoloration, thickening of the skin, and in severe cases, venous ulcers that are slow to heal.
CVI is not limited to a specific region or demographic. It affects men and women globally, though women are slightly more prone due to hormonal influences and pregnancy-related vascular changes. Risk factors such as prolonged standing, obesity, aging, genetic predisposition, and previous deep vein thrombosis contribute to its widespread occurrence.
A Widespread Yet Underrecognized Global Condition
Globally, chronic venous disorders affect a significant portion of the adult population. In many industrialized nations, studies suggest that up to 40 percent of adults show some degree of venous insufficiency. However, the true global burden may be even higher due to underreporting and limited access to vascular diagnostics in low- and middle-income countries.
One of the key reasons CVI remains overlooked is its slow progression. Symptoms often develop gradually and are initially attributed to fatigue, aging, or minor circulation issues. Patients may delay seeking care until discomfort becomes severe or complications arise.
In resource-limited settings, the problem is compounded by restricted access to vascular specialists and diagnostic tools such as duplex ultrasound imaging. As a result, many individuals live with untreated venous disease for years, increasing the risk of complications and reducing overall quality of life.
The Human Impact of Chronic Venous Insufficiency
While CVI is rarely life-threatening in its early stages, its long-term consequences can be profound. Persistent leg pain and swelling interfere with mobility and daily activities. Skin changes such as hyperpigmentation and lipodermatosclerosis can cause discomfort and emotional distress. Venous ulcers, among the most severe complications, are painful, prone to infection, and notoriously difficult to treat.
Beyond physical symptoms, CVI affects psychological well-being. Visible varicose veins and skin changes may lead to self-consciousness and reduced social participation. Chronic pain and limited mobility can contribute to decreased productivity and economic hardship.
In many parts of the world, individuals who rely on physically demanding jobs face heightened challenges. Workers who spend long hours standing or performing manual labor may experience worsening symptoms, yet may not have the flexibility or financial resources to seek early intervention.
Economic and Healthcare System Burden
From a public health perspective, Chronic Venous Insufficiency imposes significant economic strain. Advanced cases requiring wound care, surgical intervention, or hospitalization increase healthcare expenditures. Venous ulcers alone account for substantial costs due to prolonged treatment durations and recurrence rates.
Indirect costs also accumulate through lost productivity, disability, and reduced workforce participation. As populations age globally, the prevalence of CVI is expected to rise, further amplifying the economic impact.
Preventive strategies and early treatment can significantly reduce these burdens. However, achieving this requires greater awareness among both healthcare providers and the general public.
Diagnosis and Advancements in Treatment
Early diagnosis plays a crucial role in preventing complications. Duplex ultrasound remains the gold standard for evaluating venous valve function and identifying reflux. Increased availability of non-invasive imaging has improved diagnostic accuracy in many healthcare settings.
Treatment approaches have evolved considerably over the past two decades. Conservative management typically includes compression therapy, lifestyle modifications such as weight management and regular physical activity, and leg elevation. For more advanced cases, minimally invasive procedures have transformed patient outcomes.
Endovenous laser therapy, radiofrequency ablation, and sclerotherapy offer effective alternatives to traditional vein stripping surgery. These procedures are performed on an outpatient basis, involve minimal downtime, and demonstrate high success rates.
Access to specialized care is essential for optimal outcomes. Facilities such as Elite Vein Clinic provide comprehensive vascular evaluations and modern treatment options tailored to individual patient needs. Specialized centers play a vital role in bridging the gap between early symptom recognition and effective intervention.
Prevention and Public Health Strategies
Prevention remains one of the most powerful tools in addressing CVI as a global health issue. Public health campaigns that promote physical activity, weight management, and regular movement during prolonged sitting or standing can reduce risk factors associated with venous disease.
Workplace policies also have a role to play. Encouraging periodic movement breaks and ergonomic support can mitigate venous pressure in occupations that require long periods of immobility. Education initiatives aimed at primary care providers can enhance early recognition and timely referrals.
Community-level awareness is equally important. Many individuals are unaware that symptoms such as persistent leg swelling or visible vein changes warrant medical evaluation. Reducing stigma and misconceptions surrounding venous disorders can encourage earlier consultation.
Global Disparities in Care Access
Despite advances in treatment, disparities in access to vascular care remain significant. In high-income countries, minimally invasive procedures are widely available. In contrast, many regions lack trained specialists or adequate infrastructure for advanced venous interventions.
International health organizations and local governments must consider vascular health within broader chronic disease strategies. Integrating venous disease screening into primary care systems can help identify at-risk individuals earlier. Telemedicine and mobile diagnostic units may also expand access in underserved areas.
Addressing these disparities is not only a matter of medical equity but also economic sustainability. Early intervention reduces long-term complications and associated costs.
The Role of Lifestyle and Long-Term Management
While procedural interventions can correct faulty veins, long-term management often requires lifestyle adjustments. Maintaining a healthy weight reduces pressure on lower extremity veins. Regular walking enhances calf muscle pump function, which supports venous return. Elevating the legs periodically throughout the day can alleviate symptoms.
Patients benefit from understanding that CVI is a chronic condition requiring ongoing attention. Education empowers individuals to recognize symptom progression and adhere to recommended therapies such as compression garments.
Healthcare providers must emphasize continuity of care and follow-up to prevent recurrence and monitor treatment effectiveness.
Raising Global Awareness
Chronic Venous Insufficiency deserves greater recognition within global health discussions. Although it may not command the same attention as cardiovascular disease or diabetes, its prevalence and impact are substantial. Improved awareness can drive earlier diagnosis, reduce complications, and alleviate healthcare system burdens.
Educational initiatives targeting both the public and healthcare professionals are essential. Media campaigns, community health programs, and professional training workshops can help shift perceptions and encourage proactive care.
Global health frameworks increasingly emphasize comprehensive chronic disease management. Including venous disorders within these frameworks ensures a more holistic approach to vascular health.
Conclusion
Chronic Venous Insufficiency is far more than a cosmetic issue. It is a widespread vascular condition with meaningful physical, psychological, and economic consequences. As global populations age and sedentary lifestyles become more common, the prevalence of CVI is likely to rise.
Addressing this overlooked health issue requires a multifaceted approach that includes prevention, early diagnosis, access to modern treatment, and patient education. Specialized centers such as Elite Vein Clinic demonstrate how advanced, patient-centered care can improve outcomes and quality of life.
By elevating awareness and integrating venous health into broader chronic disease strategies, healthcare systems worldwide can reduce the burden of Chronic Venous Insufficiency and support healthier, more active communities.